⚠️ Affiliate Disclaimer: This post may contain affiliate links, which means I may earn a small commission at no extra cost to you, if you make a purchase through one of these links. I only recommend products or services I genuinely trust and believe can provide value. Thank you for supporting My Medical Muse!
Hormonal Headaches: 9 Powerful Causes and Proven Ways to Stop the Pain
Headaches are among the most common neurological complaints worldwide. For many women, however, headaches are not random events, they follow a pattern that aligns with hormonal shifts throughout the menstrual cycle, pregnancy, or menopause. These are known as hormonal headaches.
Hormonal headaches can be frustrating because they often appear at predictable times yet feel difficult to control. Some women experience mild discomfort, while others face intense, recurring pain that interferes with work, relationships, and daily life.
Understanding how hormones influence the brain is the first step toward managing these headaches effectively. Once you recognize the biological triggers, you can begin using strategies that reduce frequency, lessen severity, and restore control over your health.
This guide explains the science behind hormonal headaches, the symptoms to watch for, and practical ways to manage them.
What Are Hormonal Headaches?
Hormonal headaches are headaches triggered by fluctuations in reproductive hormones, particularly estrogen. These headaches are closely tied to the body’s hormonal rhythm and often appear at specific times during a woman’s life or menstrual cycle.
Hormones do far more than regulate reproduction. They influence many systems throughout the body, including brain chemistry, blood vessels, inflammation levels, and the way the nervous system processes pain. Because of this broad influence, even small hormonal shifts can affect how the brain responds to internal and external stress signals.
Estrogen plays a particularly important role in this process. It helps regulate neurotransmitters, supports healthy blood vessel function, and influences the brain’s sensitivity to pain. When estrogen levels rise or fall rapidly, these systems can temporarily become unstable. The result is often a headache.
Hormonal headaches are not random. They usually occur during predictable hormonal transitions such as:
The menstrual cycle
Pregnancy
Perimenopause
Menopause
Hormonal contraceptive use
Hormone replacement therapy
Many hormonal headaches resemble migraines rather than simple tension headaches. They may involve intense, throbbing pain that affects one side of the head, often accompanied by additional neurological symptoms.
Common features of hormonal headaches may include:
Pulsating or throbbing head pain
Sensitivity to light or sound
Nausea or vomiting
Visual disturbances such as flashing lights or blurred vision
Fatigue or brain fog
For some women, these headaches occur occasionally. For others, they appear consistently during specific hormonal phases each month. Understanding this pattern is one of the most important steps toward identifying and managing hormonal headaches effectively.
The Hormonal Headache Connection
To understand hormonal headaches more deeply, it is helpful to examine how estrogen interacts with the brain and nervous system.
The brain is extremely sensitive to hormonal signals. Estrogen receptors exist throughout key regions of the brain involved in pain processing, mood regulation, and blood flow. When hormone levels change, these areas respond almost immediately.
Estrogen influences several important neurological processes that can affect headache development.
1. Pain Regulation
Estrogen plays a significant role in regulating neurotransmitters, the chemical messengers that allow brain cells to communicate with each other.
Two important neurotransmitters influenced by estrogen are serotonin and dopamine.
Serotonin helps regulate mood, sleep, and pain perception. Dopamine affects motivation, reward pathways, and neurological balance. When estrogen levels fluctuate, these neurotransmitters can shift as well.
A sudden drop in estrogen often leads to reduced serotonin activity. Lower serotonin levels can increase the brain’s sensitivity to pain signals and trigger migraine pathways.
This explains why headaches frequently appear during times when estrogen drops quickly, such as right before menstruation.
2. Blood Vessel Function
The brain relies on a precise balance of blood flow to function properly. Estrogen helps regulate the dilation and constriction of blood vessels throughout the body, including those supplying the brain.
When estrogen levels change suddenly, blood vessels may respond unpredictably. They may expand or constrict more dramatically than usual, which can stimulate nearby pain-sensitive nerves.
This vascular response is one of the reasons migraines often involve throbbing or pulsating pain. The sensation reflects changes in blood vessel activity within the brain.
Hormonal shifts can therefore create conditions where blood vessel instability triggers headache symptoms.
3. Inflammation
Hormones also influence the body’s inflammatory response.
Estrogen generally has anti-inflammatory effects, when estrogen levels decline, inflammatory chemicals in the body may increase. These chemicals can irritate nerve endings around the brain’s blood vessels.
Inflammation in these areas activates the trigeminal nerve system, which is heavily involved in migraine pain. Once this system is activated, the brain interprets the signal as a headache.
In simple terms, hormonal fluctuations can make the brain temporarily more vulnerable to inflammation and pain signals.
Menstrual Headaches
One of the most common forms of hormonal headaches occurs around menstruation. These are often referred to as menstrual headaches or menstrual migraines.
Menstrual migraines are strongly linked to the hormonal changes that occur at the end of the menstrual cycle.
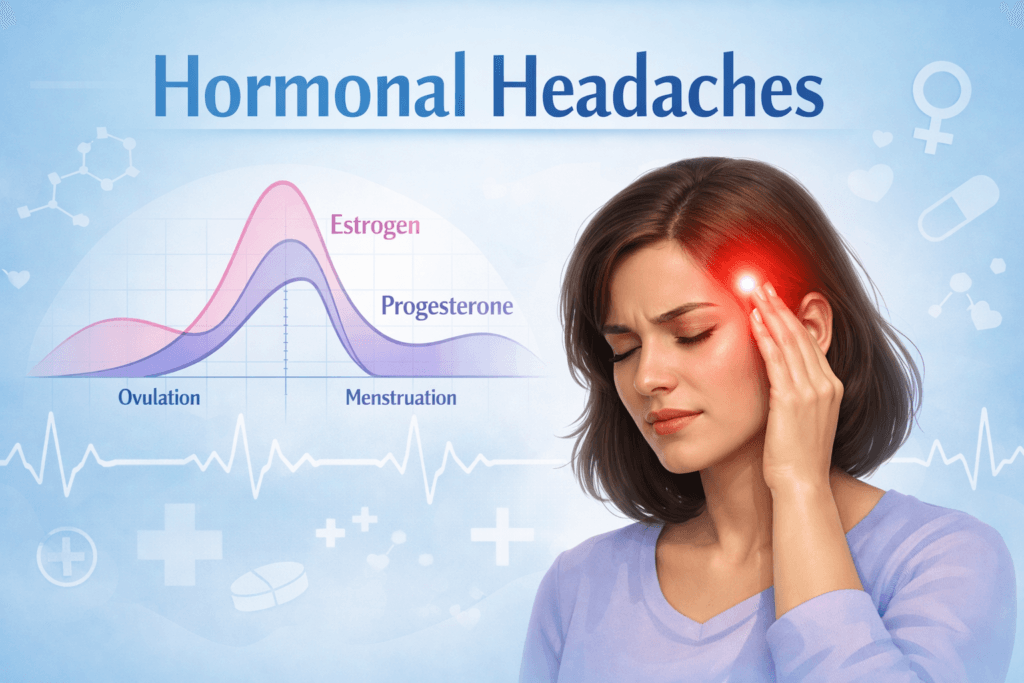
Throughout most of the cycle, estrogen levels gradually rise. However, in the days leading up to menstruation, estrogen levels drop sharply. This sudden hormonal decline can trigger migraine pathways in the brain.
Menstrual headaches typically appear within a specific time window, they most often occur:
Two days before a menstrual period begins
During the first two to three days of menstruation
Because the trigger is hormonal, the timing of these headaches is often very consistent from month to month.
Symptoms
Menstrual headaches frequently resemble migraines rather than simple tension headaches. In many cases they are more severe and longer lasting than other headaches.
Common symptoms may include:
Throbbing or pulsating pain, usually on one side of the head
Sensitivity to light and sound
Nausea or vomiting
Extreme fatigue or low energy
Neck stiffness or shoulder tension
Difficulty concentrating
Menstrual migraines also tend to last longer than typical migraines. Some may persist for several days if not treated early.
In addition, these headaches can occur alongside other premenstrual symptoms such as mood changes, bloating, breast tenderness, or sleep disturbances. This combination can make the days surrounding menstruation particularly challenging for some women.
Ovulation Headaches
Not all hormonal headaches occur before a menstrual period. Some women experience headaches around ovulation, which occurs roughly midway through the menstrual cycle.
Ovulation usually happens around day fourteen in a typical twenty eight day cycle, though the exact timing varies from person to person.
During this phase, estrogen levels rise rapidly to prepare the body for ovulation. Shortly after the egg is released, estrogen begins to decline again. This rapid rise followed by a sudden drop can trigger headaches in individuals who are sensitive to hormonal fluctuations.
Ovulation headaches may feel similar to menstrual headaches but tend to occur earlier in the cycle, some women notice a predictable headache around the same day each month when ovulation occurs.
These headaches may also appear alongside other ovulation-related changes in the body.
Common ovulation symptoms include:
Mild pelvic discomfort or lower abdominal pain
Increased cervical mucus with a clear, stretchy texture
A slight increase in basal body temperature
Breast tenderness
Heightened sense of smell or sensitivity
Because ovulation is hormonally driven, headaches during this phase often follow a consistent pattern. Women who track their menstrual cycles sometimes notice that headaches appear at the same point every month.
Recognizing this pattern can be extremely helpful. Once ovulation headaches are identified, preventive strategies can be used during that specific window of the cycle.
Over time, this awareness allows individuals to better anticipate symptoms and manage hormonal headaches before they become severe.
Headaches During Pregnancy
Pregnancy causes dramatic hormonal shifts, especially during the first trimester.
Estrogen and progesterone levels rise rapidly, which can affect blood flow and neurotransmitter activity.
Some women notice that headaches become more frequent early in pregnancy. Others find that migraines improve, especially later in pregnancy.
Common triggers for headaches during pregnancy include:
Hormonal changes
Fatigue
Dehydration
Low blood sugar
Stress
While most pregnancy headaches are harmless, severe headaches should always be discussed with a healthcare provider.
Hormonal Headaches During Perimenopause
Perimenopause is the transitional phase leading up to menopause, and it is one of the most hormonally unstable periods in a woman’s life. This stage can begin several years before menopause and is characterized by unpredictable fluctuations in estrogen and progesterone levels.
Unlike the relatively structured hormonal pattern seen during the reproductive years, perimenopause introduces irregular hormonal shifts. Estrogen may surge dramatically one month and drop sharply the next, these abrupt hormonal swings can significantly affect the brain’s pain pathways, making headaches more likely.
For many women, perimenopause is the first time they begin experiencing migraines or recurring headaches. Others who previously had occasional headaches may notice that they become more frequent, more intense, or more difficult to control.
Several mechanisms contribute to headaches during this stage. Rapid estrogen changes can alter serotonin levels, disrupt blood vessel regulation, and increase inflammatory activity around nerve pathways associated with migraine pain.
As a result, women in perimenopause may experience a range of symptoms that accompany hormonal headaches.
Common symptoms during this stage may include:
More frequent headaches throughout the month
Migraines that last longer than usual
Increased sensitivity to light, sound, or strong smells
Headaches that occur alongside hot flashes
Sleep disturbances that worsen headache severity
Brain fog or difficulty concentrating
Sleep disruption is especially important during perimenopause. Hormonal changes can interfere with sleep quality, and poor sleep is a known trigger for migraines. When hormonal instability combines with sleep deprivation, headaches may become more persistent.
The good news is that for many women, headaches improve after menopause. Once menstruation stops and estrogen levels stabilize at a lower level, the extreme hormonal swings responsible for many migraines gradually disappear.
However, this improvement does not occur for everyone, some women may continue experiencing headaches due to other triggers such as stress, sleep patterns, diet, or underlying migraine disorders.
Understanding the connection between hormonal transitions and headaches can help women prepare for this stage and seek appropriate treatment when necessary.
Hormonal Birth Control and Headaches
Hormonal contraceptives can have complex effects on headaches. For some women, they reduce headache frequency by stabilizing hormone levels. For others, they may trigger migraines or make existing headaches worse.
Hormonal birth control methods include options such as oral contraceptive pills, patches, vaginal rings, hormonal injections, and certain intrauterine devices. These methods typically contain synthetic versions of estrogen, progesterone, or both.
Birth control pills work by regulating the menstrual cycle and preventing ovulation. By delivering controlled doses of hormones, they reduce the natural fluctuations that occur during the menstrual cycle. In some individuals, this hormonal stability helps prevent headaches.
However, headaches may still occur in several situations, common scenarios where hormonal contraceptives may trigger headaches include:
During the placebo or hormone-free week of birth control pills
When starting a new contraceptive method
When switching between different hormonal formulations
If estrogen levels drop suddenly during the cycle
The placebo week is particularly important, during this time, hormone levels temporarily decline, which can mimic the estrogen drop that occurs before menstruation. This drop can trigger headaches in women who are sensitive to hormonal changes.
Another important consideration involves migraines with aura. Migraine aura refers to neurological symptoms that appear before the headache begins, such as visual disturbances, flashing lights, or temporary blind spots.
Women who experience migraines with aura should consult a healthcare professional before using estrogen-containing contraceptives. In certain cases, estrogen-based birth control may increase the risk of stroke, especially when combined with other risk factors such as smoking or high blood pressure.
Because every individual responds differently to hormonal contraception, finding the right method may require some trial and adjustment. A healthcare provider can help evaluate options based on medical history, headache patterns, and overall health.
Recognizing Hormonal Headache Patterns
One of the most effective ways to understand hormonal headaches is to track them over time. Many women discover that their headaches follow a predictable pattern when compared with their menstrual cycle or other hormonal events.
Keeping a headache diary can provide valuable insights into these patterns. By documenting headaches consistently, it becomes easier to identify whether symptoms are linked to hormonal changes or other lifestyle factors.
A useful headache diary should include several key details.
Important information to record includes:
The date and time the headache begins
The stage of the menstrual cycle
The severity and duration of the headache
Associated symptoms such as nausea or light sensitivity
Food and drink consumed before the headache
Sleep quality the night before
Stress levels during the day
Physical activity or exercise
Over several weeks or months, clear trends often begin to emerge. For example, headaches may appear consistently one or two days before menstruation, during ovulation, or after nights of poor sleep.
Recognizing these patterns allows individuals to anticipate potential headaches and take preventive steps ahead of time. Preventive strategies may include adjusting sleep schedules, increasing hydration, reducing stress, or taking medications early when symptoms begin.
This proactive approach often leads to better headache control and improved quality of life.
Common Triggers That Worsen Hormonal Headaches
Hormonal fluctuations may initiate headaches, but they are rarely the only factor involved. Many lifestyle and environmental triggers can intensify hormonal headaches or make them occur more frequently.
Understanding these triggers is essential because managing them can significantly reduce the overall burden of headaches.
1. Stress
Stress is one of the most powerful headache triggers. When the body experiences stress, it releases hormones such as cortisol and adrenaline. These chemicals prepare the body for a fight-or-flight response but can also increase muscle tension and alter blood flow in the brain.
Chronic stress may amplify the sensitivity of pain pathways already affected by hormonal changes, making headaches more intense and harder to control.
2. Sleep Disruption
Sleep plays a crucial role in regulating hormonal balance and brain function. Irregular sleep schedules, insomnia, or poor sleep quality can disrupt the body’s natural rhythms.
When sleep is inadequate, the brain becomes more vulnerable to inflammation and pain signals. This vulnerability can significantly worsen hormonal headaches.
3. Dehydration
Even mild dehydration can trigger headaches. The brain depends on adequate hydration to maintain proper blood circulation and cellular function.
Hormonal shifts may make individuals more sensitive to dehydration, meaning headaches may occur more easily if fluid intake is insufficient.
4. Caffeine Changes
Caffeine affects blood vessel activity in the brain, a sudden increase or decrease in caffeine intake can trigger headaches, particularly when combined with hormonal fluctuations.
Consistent caffeine habits are generally less likely to provoke headaches than dramatic changes in daily consumption.
5. Skipped Meals
Low blood sugar can also trigger headaches. When meals are skipped or delayed, glucose levels fall and the brain may struggle to maintain stable energy.
Combined with hormonal changes, this drop in blood sugar can increase headache risk. Managing these triggers through lifestyle adjustments can make a significant difference in reducing headache frequency and severity.
Natural Ways to Manage Hormonal Headaches
Lifestyle changes are often the first line of defense against hormonal headaches. While they may not eliminate headaches entirely, they can reduce their intensity and make them easier to manage.
1. Maintain Stable Blood Sugar
Eating balanced meals at regular intervals helps maintain stable energy levels and supports hormone regulation. Long gaps between meals can lead to blood sugar fluctuations that trigger headaches.
A balanced meal typically includes:
Protein to support muscle and brain function
Fiber to slow digestion and stabilize blood sugar
Healthy fats for sustained energy
Complex carbohydrates for gradual glucose release
This combination helps maintain steady energy throughout the day.
2. Stay Hydrated
Adequate hydration supports circulation and helps maintain proper brain function. Dehydration can worsen headaches and increase fatigue.
Drinking water regularly throughout the day is a simple yet effective strategy for preventing headaches.
3. Improve Sleep Quality
Establishing consistent sleep routines can significantly reduce headache frequency. Going to bed and waking up at the same time each day helps regulate circadian rhythms and hormonal balance. Most adults benefit from seven to nine hours of sleep per night.
4. Exercise Regularly
Physical activity improves circulation, reduces stress hormones, and supports overall hormonal balance. Moderate exercise has also been shown to reduce the frequency of migraines in some individuals.
Helpful activities include:
Walking
Cycling
Swimming
Yoga
Stretching exercises
Regular movement also promotes better sleep and stress management.
5. Manage Stress
Stress management techniques can play a major role in preventing hormonal headaches.
Effective approaches may include:
Deep breathing exercises
Meditation or mindfulness practice
Gentle stretching or yoga
Journaling
Spending time in relaxing environments
Reducing daily stress helps prevent the neurological overstimulation that often contributes to headaches.
Nutritional Support for Hormonal Headaches
Certain nutrients may help support brain health and reduce the likelihood of migraines associated with hormonal fluctuations.
1. Magnesium
Magnesium is essential for proper nerve signaling and blood vessel regulation. It helps relax blood vessels and supports healthy muscle function.
Research has linked low magnesium levels to increased migraine frequency. Ensuring adequate magnesium intake may reduce headache risk for some individuals.
Foods rich in magnesium include:
Almonds
Spinach
Pumpkin seeds
Avocados
Whole grains
2. Riboflavin (Vitamin B2)
Riboflavin plays an important role in cellular energy production. Brain cells require a large amount of energy to function properly, and riboflavin helps support the mitochondria that produce this energy.
Some studies suggest that riboflavin supplementation may reduce migraine frequency.
3. Omega-3 Fatty Acids
Omega-3 fatty acids have strong anti-inflammatory properties and support cardiovascular health. By reducing inflammation and stabilizing blood vessels, omega-3s may help decrease headache intensity.
Common sources of omega-3s include:
Fatty fish such as salmon and sardines
Walnuts
Flaxseeds
Chia seeds
Before beginning any supplement regimen, it is best to consult a healthcare professional to ensure safety and proper dosage.
Medical Treatments for Hormonal Headaches
When lifestyle strategies are not enough, medical treatment may be necessary to control severe or persistent headaches.
1. Pain Relievers
Over-the-counter pain relievers are often the first step in treating hormonal headaches.
Common options include:
Acetaminophen
Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or naproxen
These medications are generally most effective when taken early in the headache cycle, before the pain becomes severe.
2. Migraine Medications
For individuals with frequent migraines, doctors may prescribe medications specifically designed to treat migraine attacks.
One commonly used group of medications is triptans. These drugs work by targeting serotonin receptors in the brain, helping reduce inflammation and constrict overactive blood vessels.
When taken at the first sign of a migraine, triptans can significantly shorten the duration of symptoms.
3. Hormonal Therapy
In some cases, stabilizing hormone levels may help prevent recurring headaches. Hormonal therapy may be recommended when headaches are strongly linked to menstrual or perimenopausal changes.
Possible options include:
Continuous birth control pills to prevent hormone withdrawal
Estrogen patches during certain phases of the menstrual cycle
Hormone replacement therapy during menopause
Treatment decisions depend on individual medical history, risk factors, and the severity of symptoms.
When Hormonal Headaches Might Signal a Bigger Problem
Most hormonal headaches are not dangerous and can be managed effectively. However, certain symptoms may indicate a more serious underlying condition.
Medical evaluation is recommended if headaches:
Appear suddenly with extreme intensity
Occur alongside confusion or difficulty speaking
Cause weakness or numbness on one side of the body
Wake you from sleep regularly
Feel significantly different from previous headaches
These symptoms could signal neurological or vascular problems that require immediate medical attention.
Prompt medical assessment helps ensure that serious conditions are identified early and treated appropriately.
Long Term Outlook
Hormonal headaches often follow recognizable patterns that correspond with the body’s natural hormonal cycles. Once these patterns are understood, many individuals can significantly reduce headache frequency through lifestyle adjustments and targeted treatments.
For some women, headaches improve naturally after menopause as hormonal fluctuations become less dramatic. For others, managing lifestyle triggers, optimizing sleep, maintaining balanced nutrition, and using appropriate medications provides long-term relief.
The most effective approach combines awareness with proactive care. By paying attention to the body’s signals and responding early, hormonal headaches can become far less disruptive and much easier to control over time.
Final Thoughts
Hormonal headaches are not random discomforts or unexplained pain, they are the brain’s response to powerful hormonal shifts that naturally occur throughout a woman’s life. From the menstrual cycle to pregnancy, perimenopause, and menopause, these hormonal transitions influence the delicate systems that regulate pain, blood flow, and brain chemistry.
Understanding this connection changes the way hormonal headaches are viewed. Instead of feeling unpredictable or mysterious, they begin to reveal patterns. When those patterns become clear, it becomes much easier to anticipate symptoms and respond early rather than feeling caught off guard each time a headache appears.
Tracking your menstrual cycle, paying attention to lifestyle triggers, and observing how your body responds to hormonal changes can provide valuable insights. Over time, this awareness allows you to recognize the warning signs before a headache fully develops. Small adjustments such as improving sleep, maintaining regular meals, managing stress, and staying hydrated can make a meaningful difference in reducing the frequency and severity of these headaches.
For women whose headaches remain severe or disruptive, medical care can offer additional support. Healthcare professionals can help identify hormonal patterns, recommend appropriate treatments, and rule out other underlying causes, with the right guidance, many people find strategies that bring significant relief.
The most important thing to remember is that hormonal headaches are manageable. They may be influenced by natural biological changes, but they do not have to dictate your daily life, with the right knowledge, awareness of your body’s signals, and a proactive approach to prevention and treatment, hormonal headaches can become far less overwhelming.
Understanding your body is a powerful tool, when you learn how hormones affect your brain and recognize the rhythms behind your symptoms, you gain the ability to respond with confidence instead of frustration. Over time, that knowledge can transform hormonal headaches from a recurring disruption into a condition that is predictable, manageable, and far less intrusive in your life.
👩⚕️ Need Personalized Health Advice?
Get expert guidance tailored to your unique health concerns through MuseCare Consult. Our licensed doctors are here to help you understand your symptoms, medications, and lab results—confidentially and affordably.
👉 Book a MuseCare Consult NowRecommended Reads:
- PMS vs PMDD: 9 Critical Differences Every Woman Must Know
- 7 Proven Ways to Relieve Back Pain During Ovulation Naturally
- Dizziness During Period: 9 Real Causes Every Woman Should Know
- 7 Proven Ways to Beat Fatigue Before Period: Stop Feeling Drained Every Month
- Period Pain Worse Some Months: 9 Shocking Reasons Your Cramps Change
- 13 Real Reasons You Get Severe Cramps but Normal Period (What to Do Next)
- Menstrual Cycle Related Symptoms: 21 Normal Signs vs Dangerous Red Flags Every Woman Must Know
Dr. Ijasusi Bamidele, MBBS (Binzhou Medical University, China), is a medical doctor with 5 years of clinical experience and founder of MyMedicalMuse.com, a subsidiary of Delimann Limited. As a health content writer for audiences in the USA, Canada, and Europe, Dr. Ijasusi helps readers understand complex health conditions, recognize why they have certain symptoms, and apply practical lifestyle modifications to improve well-being


